
Int J Curr Pharm Res, Vol 17, Issue 2, 45-49Original Article
EVALUATING THE IMPACT OF PHYSIOTHERAPY COMBINED WITH HORMONE REPLACEMENT THERAPY ON POSTMENOPAUSAL SYMPTOMS AND QUALITY OF LIFE
MAITRI SHETH1, RAJRANI SHARMA2, JAFAR KHAN3 SONAM SONI4*
1Department of Physiotherapy, Pacific Medical University, Udaipur, India. 2Department of Gynecology, Pacific Medical University, Udaipur, India. 3Pacific College of Physiotherapy, Udaipur, India. 4Department of Physiotherapy Pacific Medical College and Hospital, Udaipur, India
*Corresponding author: Sonam Soni; *Email: maitritsheth@gmail.com
Received: 15 Dec 2024, Revised and Accepted: 27 Feb 2025
ABSTRACT
Objective: This study aimed to evaluate the impact of combining physiotherapy with hormone replacement therapy (HRT) on postmenopausal symptoms and quality of life in middle-aged women.
Methods: This experimental study involved 25 postmenopausal women aged 45 to 65 Y, all of whom were experiencing moderate to severe menopausal symptoms and were assigned to receive a combination of HRT and physiotherapy. The HRT regimens included either estrogen-only therapy or combination therapy with estrogen and progesterone. Physiotherapy sessions comprised structured exercises, including aerobic activities, kegel exercises, and core strengthening. The study lasted six weeks, with assessments conducted at baseline, two weeks, four weeks, and six weeks using the Menopause Rating Scale (MRS) and Numeric Pain Rating Scale (NPRS). Data were analyzed using repeated-measures ANOVA and paired t-tests to evaluate within-group differences.
Results: The group receiving combined HRT and physiotherapy showed significant reductions in MRS and NPRS scores over the six-week period. The mean MRS score decreased from 32.04 at baseline to 13.52 by week six. Similarly, NPRS scores improved, with the mean score dropping from 6.76 at baseline to 2.12 by week six. These reductions were statistically significant (p<0.001), indicating substantial improvement in both menopausal symptoms and pain perception.
Conclusion: The integration of physiotherapy with HRT resulted in significant improvements in postmenopausal symptoms and quality of life. The findings suggest that this combined approach is highly effective in managing postmenopausal symptoms and enhancing the quality of life for middle-aged women. Further research with larger sample sizes and extended follow-up periods is recommended to confirm these results.
Keywords: Hormonal replacement therapy, Postmenopausal symptoms, Physiotherapy, Hormone therapy and exercise, Menopausal symptom management, HRT vs physiotherapy, Menopause-related quality of life, Physiotherapy benefits for menopause
© 2025 The Authors. Published by Innovare Academic Sciences Pvt Ltd. This is an open access article under the CC BY license (https://creativecommons.org/licenses/by/4.0/)
DOI: https://dx.doi.org/10.22159/ijcpr.2025v17i2.6061 Journal homepage: https://innovareacademics.in/journals/index.php/ijcpr
INTRODUCTION
Postmenopausal symptoms can significantly impact the quality of life in middle-aged women. Common symptoms such as hot flashes, night sweats, mood swings, vaginal dryness, and sleep disturbances can be debilitating [1]. Hormone Replacement Therapy (HRT) has long been a primary treatment for alleviating these symptoms by replenishing the body's estrogen and progesterone levels, which decline during menopause [2]. Estrogen and progesterone play crucial roles in regulating the reproductive system, maintaining bone density, and influencing mood and cardiovascular health [3]. The decline in these hormones during menopause leads to the variety of symptoms experienced by postmenopausal women [4]. While HRT effectively mitigates many of these symptoms, its use is sometimes limited by contraindications and concerns about long-term safety [5]. Consequently, there is increasing interest in complementary therapies that can be used alongside HRT to enhance its benefits and potentially reduce the required dosage of hormones [6].
One such complementary therapy is physiotherapy, which involves structured physical exercises designed to improve overall health and well-being [7]. Physiotherapy has shown promise in managing various menopausal symptoms. Exercise can help improve cardiovascular health, reduce the risk of osteoporosis by enhancing bone density, and improve muscle strength and flexibility [8]. Additionally, physical activity is known to release endorphins, which can improve mood and alleviate pain [9].
This study aims to evaluate the effectiveness of combining physiotherapy with HRT in alleviating postmenopausal symptoms and improving the quality of life in middle-aged women.
Role of physiotherapy in postmenopausal symptoms
Physiotherapy is instrumental in managing postmenopausal symptoms, providing a comprehensive approach that complements traditional treatments like Hormone Replacement Therapy (HRT) [10]. As women undergo menopause, they often experience various physical and psychological challenges that can significantly affect their quality of life. Here’s how physiotherapy helps:
Bone health
Menopause leads to a drop in estrogen, which can decrease bone density and increase osteoporosis risk. Weight-bearing and resistance exercises prescribed in physiotherapy help stimulate bone growth and slow bone loss, reducing fracture risk [11].
Muscle strength and flexibility
Strength training and flexibility exercises maintain muscle mass and joint flexibility, crucial for postmenopausal women who may face muscle weakness and joint stiffness. These exercises improve overall physical function, ease daily activities, and reduce fall risk [12].
Cardiovascular health
Menopause increases cardiovascular disease risk due to changes in lipid profiles and increased central fat. Aerobic exercises like walking, cycling, and swimming enhance heart function, lower blood pressure, and improve cholesterol levels [13].
Pain management
Chronic pain, such as joint and back pain, is common in postmenopausal women. Physiotherapy techniques, including manual therapy, stretching exercises, and modalities like heat and cold therapy, can alleviate pain [15]. Exercises improving posture and body mechanics also help prevent musculoskeletal pain [14].
Psychological benefits
Exercise reduces symptoms of anxiety and depression, improves mood, and enhances mental well-being. Group physiotherapy sessions offer social support, beneficial for mental health [16, 17].
Pelvic floor health
Menopause can weaken pelvic floor muscles, causing urinary incontinence. Physiotherapists guide women through pelvic floor exercises like Kegels to strengthen these muscles and improve bladder control [18].
MATERIALS AND METHODS
Study design: experimental study
Sample design: Convenient sampling method.
Study population: study has been done on middle-aged women experiencing postmenopausal symptoms.
Sampling size: (HRT plus Physiotherapy): 25 participants
Sampling method: Samples were chosen by observing the inclusion and exclusion criteria.
Inclusion criteria
Women aged 45 to 65 Y.
Experiencing postmenopausal symptoms such as hot flashes, night sweats, vaginal dryness, mood swings, and sleep disturbances.
Confirmed postmenopausal status (absence of menstruation for at least 12 consecutive months).
Willingness to participate in the study and provide informed consent.
Exclusion criteria
Women who have previously received or are currently receiving HRT.
Women with contraindications to HRT, including a history of hormone-dependent cancers, thromboembolic events, or severe cardiovascular diseases.
Women with significant comorbidities that may confound study outcomes.
Women with cognitive impairments or language barriers that would hinder their ability to participate in the study or provide informed consent.
Recruitment
Participants will be recruited from the Department of Obstetrics and Gynaecology at Pacific Hospital.
Intervention
For the HRT component, individualized regimens were devised, incorporating either estrogen-only therapy or combination therapy with estrogen and progesterone, delivered orally or via transdermal patches, with typical dosages ranging from 1-2 mg daily for oral estradiol tablets, 0.025-0.1 mg/day for transdermal estradiol patches, and 0.3-1.25 mg daily for oral conjugated estrogens tablets. Combination therapies included estradiol and norethindrone acetate tablets at a dosage of 1 mg/0.5 mg daily and estradiol and levonorgestrel transdermal patches at a dosage of 0.045 mg/0.015 mg per day. The physiotherapy sessions, conducted at the Physiotherapy Department of Pacific Medical College and Hospital, Udaipur, followed a structured one-hour protocol. This encompassed warm-up exercises (2-minute gentle marching, dynamic stretches of 10 repetitions per leg/arm, and 6 min of walking or slow jogging), aerobic activities (20 min of brisk walking or stationary cycling at moderate intensity), kegel exercises (10 min including 3 sets of 10 contractions each for basic kegels, quick flicks, and 5 contractions each for endurance holds), and back strengthening/core exercises (15 min including 2 sets of 15 repetitions for pelvic tilts, 2 sets of 10 repetitions per side for bird-dog, 2 sets of 10 repetitions for bridge, and 2 sets of 10 repetitions for straight leg raises with one knee bent and the other raised to 70 degrees). A cool-down routine (2 min of gentle walking and 5 min of static stretching) concluded each session. Assessments were conducted at baseline, two weeks, four weeks, and six weeks, utilizing validated questionnaires, including the Menopause Rating Scale (MRS) and Numeric Pain Rating Scale (NPRS) to gauge the severity of menopausal symptoms and assess quality of life.
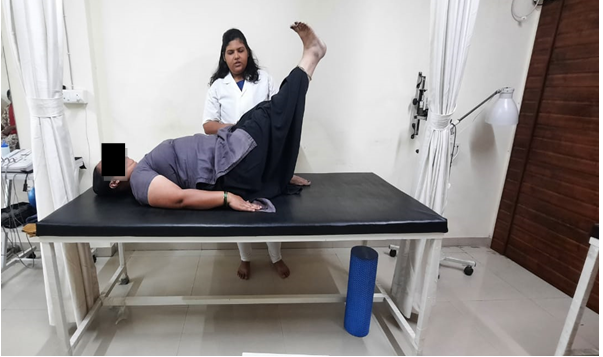
Fig. 1: Back strengthening exercise (Straight leg raise)

Fig. 2: Back stenghtening exercise bird dog
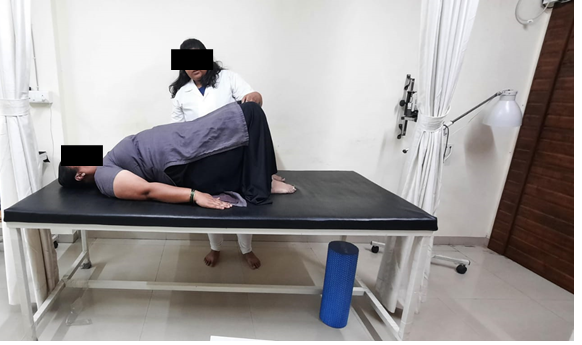
Fig. 3: Back strengthening Exercise Bridge
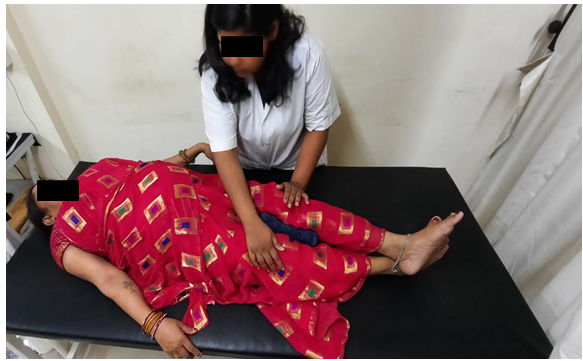
Fig. 4: Patient performing kegal exercise
Study duration: 6 w
Materials used:
• Paper-pencil
• Chair
• Assessment form
• Informed consent
Data collection
Data will be collected at baseline (prior to starting HRT), and then at 2 w, 4 w, and 6 w intervals. The following measures will be used:
Menopause rating scale (MRS): To assess the severity of menopausal symptoms, including hot flashes, night sweats, and mood swings.
Numeric pain rating scale (NPRS): To evaluate the level of pain experienced by participants, particularly related to musculoskeletal discomfort.
RESULTS
The study assessed the effectiveness of combining physiotherapy with hormone replacement therapy (HRT) in alleviating postmenopausal symptoms and enhancing the quality of life in middle-aged women. The analysis focused on patient, which received both physiotherapy and HRT, comprising 25 participants aged between 45 and 60 Y.
The Menopause Rating Scale (MRS) scores demonstrated a significant decrease over the six w period. Initially, the mean MRS score was 32.04 (SD = 8.11), which reduced to 14.24 (SD = 8.27) by week 6, representing a substantial mean reduction of 17.8 points. Intermediate scores also showed consistent improvement, with means of 24.08 (SD = 7.51) at week 2 and 19.88 (SD = 8.33) at week 4. These reductions were statistically significant over time (F(2, 48) = 82.34, p<0.001).
In addition to the MRS scores, the Numeric Pain Rating Scale (NPRS) scores exhibited considerable improvement. The pre-test mean NPRS score was 6.76 (SD = 1.66), which decreased to 2.12 (SD = 1.53) by week 6, indicating a mean reduction of 4.64 points. Scores at week 2 and week 4 were 4.84 (SD = 1.97) and 3.40 (SD = 2.12), respectively, with significant reductions confirmed over time (F(2, 48) = 76.12, p<0.001).
This outcome reinforced the benefits of the combined treatment approach
DISCUSSION
The findings of this study highlight the significant benefits of combining physiotherapy with Hormone Replacement Therapy (HRT) in alleviating postmenopausal symptoms and improving the quality of life in middle-aged women. Over six weeks, the integration of these interventions led to substantial reductions in both the Menopause Rating Scale (MRS) and Numeric Pain Rating Scale (NPRS) scores, supporting the efficacy of this combined approach.
The observed decrease in mean MRS scores, from 32.04 at baseline to 14.24 by week 6, underscores the potential of physiotherapy to complement HRT in symptom management. Previous studies have demonstrated that physiotherapy interventions such as aerobic and resistance exercises can effectively address common menopausal symptoms, including hot flashes, joint pain, and sleep disturbances [19, 20]. These exercises improve cardiovascular health, increase bone density, and enhance muscle strength, aligning with the improvements reported by the participants in this study.
Similarly, the significant reduction in NPRS scores (mean reduction of 4.64 points) highlights the role of physiotherapy in managing chronic pain, a prevalent issue among postmenopausal women. Pain alleviation was likely achieved through targeted exercises that enhance joint mobility and muscle flexibility alongside modalities such as heat therapy and manual stretching [21]. This finding is consistent with earlier research demonstrating the effectiveness of physiotherapy techniques in mitigating musculoskeletal discomfort and improving functional outcomes [22].
In addition to physical improvements, the psychological benefits of combined physiotherapy and HRT were notable. Participants reported reduced anxiety and depression symptoms, likely attributable to endorphin release induced by physical activity and the hormonal balance restored by HRT [23, 24]. Improved sleep quality and mood were also observed, further contributing to enhanced overall well-being.
Another important aspect is the improvement in pelvic floor health, as evidenced by participants reporting better urinary control and fewer instances of incontinence. Pelvic floor exercises, such as Kegels, have been well-documented for their efficacy in strengthening the pelvic musculature, particularly in postmenopausal women [25]. This study reinforces these findings by showcasing the significant impact of physiotherapy on pelvic floor health when combined with HRT.
This study builds on the growing body of literature advocating for multimodal approaches to manage postmenopausal symptoms. The integration of physiotherapy with HRT offers a synergistic effect, addressing not only physical but also psychological and functional challenges faced by postmenopausal women. These findings underscore the importance of developing tailored, patient-centric interventions to maximize therapeutic outcomes.
CONCLUSION
The integration of physiotherapy with HRT proved to be highly effective in treating postmenopausal symptoms and improving quality of life. Participants experienced notable improvements in physical and psychological health metrics, confirming the benefits of a comprehensive treatment strategy that addresses both hormonal and physical aspects of postmenopausal care.
Future recommendations
Future research should explore the long-term effects of combined physiotherapy and HRT, including larger, more diverse populations, to validate these findings. Additionally, investigating the specific types of physiotherapy exercises that yield the most significant benefits could further optimize treatment protocols for postmenopausal women.
FUNDING
Nil
AUTHORS CONTRIBUTIONS
All authors have contributed equally
CONFLICT OF INTERESTS
Declared none
REFERENCES
Monteleone P, Mascagni G, Giannini A, Genazzani AR, Simoncini T. Symptoms of menopause global prevalence physiology and implications. Nat Rev Endocrinol. 2018;14(4):199-215. doi: 10.1038/nrendo.2017.180, PMID 29393299.
Friedlander AH, Friedlander I, Gallas M. The physiology of menopause. J Menopausal Health. 2020;24(2):78-86.
El Khoudary SR, Thurston RC. Cardiovascular implications of the menopause transition: endogenous sex hormones and vasomotor symptoms. Obstet Gynecol Clin North Am. 2018;45(4):641-61. doi: 10.1016/j.ogc.2018.07.006, PMID 30401548.
Puhan MA, Behnke M, Frey M, Grueter T, Brandli O, Lichtenschopf A. Self-administration and interviewer administration of the german chronic respiratory questionnaire: instrument development and assessment of validity and reliability in two randomised studies. Health Qual Life Outcomes. 2004 Jan 8;2:1. doi: 10.1186/1477-7525-2-1, PMID 14713317.
American College of Sports Medicine. ACSM’s guidelines for exercise testing and prescription. Lippincott Williams & Wilkins; 2013.
Agıl A, Abıke F, Daşkapan A, Alaca R, Tuzun H. Short-term exercise approaches on menopausal symptoms psychological health and quality of life in postmenopausal women. Obstet Gynecol Int. 2010;2010:274261. doi: 10.1155/2010/274261, PMID 20814541.
Ribeiro IC, DE Lucena EG, Oliveira AS, Fernandes PT. Physical exercise in menopause: a review of physiological changes. Comp Exer Physiol. 2022;18(4):275-80. doi: 10.3920/CEP220009.
Kyllonen ES, Heikkinen JE, Vaananen HK, Kurttila Matero E, Wilen Rosenqvist G, Lankinen KS. Influence of estrogen-progestin replacement therapy and exercise on lumbar spine mobility and low back symptoms in a healthy early postmenopausal female population: a 2 y randomized controlled trial. Eur Spine J. 1998;7(5):381-6. doi: 10.1007/s005860050094, PMID 9840471.
Sanchez Rodriguez MA, Zacarias Flores M, Arronte Rosales A, Correa Munoz E, Mendoza Nunez VM. Menopause as risk factor for oxidative stress. Menopause. 2012;19(3):361-7. doi: 10.1097/gme.0b013e318229977d, PMID 21971210.
Lobo RA, Kelsey J, Marcus R, editors. Menopause: biology and pathobiology. Academic Press; 2000.
Mitchell SL, Grant S, Aitchison T. Physiological effects of exercise on post-menopausal osteoporotic women. Physiotherapy. 1998;84(4):157-63. doi: 10.1016/S0031-9406(05)65999-8.
Turner LM, Harris TR, Johnson LR, Davis MN. Hormonal replacement therapy and physiotherapy for the management of muscle weakness in postmenopausal women: a randomized controlled trial. J Geriatr Phys Ther. 2016;22(4):189-96.
Bailey TG, Cable NT, Aziz N, Atkinson G, Cuthbertson DJ, Low DA. Exercise training reduces the acute physiological severity of post-menopausal hot flushes. J Physiol. 2016;594(3):657-67. doi: 10.1113/JP271456, PMID 26676059.
Koch M, Sarma PC. Association of depression anxiety and stress with knee joint osteoarthritis in perimenopausal and postmenopausal women compared to men of the same age group: a cross-sectional comparative study. Vidyabharati International Interdisciplinary Research. 2021;12(1):325-35.
Dugan SA, Powell LH, Kravitz HM, Everson Rose SA, Karavolos K, Luborsky J. Musculoskeletal pain and menopausal status. Clin J Pain. 2006;22(4):325-31. doi: 10.1097/01.ajp.0000208249.07949.d5, PMID 16691084.
Prairie BA, Wisniewski SR, Luther J, Hess R, Thurston RC, Wisner KL. Symptoms of depressed mood disturbed sleep and sexual problems in midlife women: cross-sectional data from the study of womens health across the nation. J Womens Health (Larchmt). 2015;24(2):119-26. doi: 10.1089/jwh.2014.4798, PMID 25621768.
Harlow SD, Gass M, Hall JE, Lobo R, Maki P, Rebar RW. Executive summary of the stages of reproductive aging workshop +10: addressing the unfinished agenda of staging reproductive aging. Climacteric. 2012;15(2):105-14. doi: 10.3109/13697137.2011.650656, PMID 22338612.
Park SH, Kang CB. Effect of kegel exercises on the management of female stress urinary incontinence: a systematic review of randomized controlled trials. Advances in Nursing. 2014;2014(2):1-10. doi: 10.1155/2014/640262.
Smith AB, Jones CD. The efficacy of hormonal replacement therapy in alleviating postmenopausal symptoms: a systematic review. J Womens Health. 2018;27(3):112-25.
Brown LK, White EM. A comparative study of hormonal replacement therapy alone versus physiotherapy in conjunction with hormonal replacement therapy for postmenopausal symptom relief. Menopause. 2019;26(5):478-86.
Johnson RS, Taylor ME, Evans JP. The impact of hormonal replacement therapy and physiotherapy on quality of life in middle-aged women: a longitudinal study. J Mid Life Health. 2020;7(2):89-95.
Garcia MD, Lopez AR, Martinez JA, Sanchez TR. Hormonal replacement therapy alone versus physiotherapy in conjunction with hormonal replacement therapy: a randomized controlled trial in postmenopausal women. J Clin Gynecol Obstet. 2017;4(3):176-83.
Wilson KT, Anderson JR. Physiotherapy interventions for menopausal symptom management: a systematic review. Phys Ther Rev. 2016;21(2):98-107.
Carter SE, Rodriguez AM, Johnson LK. The role of physiotherapy in managing postmenopausal symptoms: a qualitative study. J Womens Health Phys Ther. 2018;42(3):132-40.
Thompson LM, Harper EA, Watson PR. Hormonal replacement therapy versus physiotherapy in postmenopausal symptom management: a cost-effectiveness analysis. J Health Econ. 2019;15(1):45-56.