
Int J Curr Pharm Res, Vol 18, Issue 1, 80-84Original Article
QUALITY OF SLEEP AND ITS RELATIONSHIP WITH DEPRESSIVE SYMPTOMATOLOGY AND SUICIDALITY IN UNIPOLAR DEPRESSION
BHASKAR ROY1, PRANAB DAS2*
1Department of Psychiatry, Burdwan Medical College and Hospital, Bardhaman, West Bengal, India. 2Department of Pharmacology, Pragjyotishpur Medical College and Hospital, Guwahati, Assam, India
*Corresponding author: Pranab Das; *Email: pranabdas2580123@gmail.com
Received: 06 Oct 2025, Revised and Accepted: 26 Nov 2025
ABSTRACT
Objective: To evaluate the relationship between sleep quality, depressive symptomatology, and suicidality among patients with unipolar depression.
Methods: This hospital-based cross-sectional study was conducted in the Department of Psychiatry, Burdwan Medical College and Hospital, West Bengal. Fifty patients aged 18–60 y, fulfilling ICD-11 criteria for Major Depressive Disorder, were recruited by simple random sampling. Clinical assessment included the Sleep Quality Scale (SQS), Beck Depression Inventory (BDI), and Columbia–Suicide Severity Rating Scale (C-SSRS). Data were analyzed using SPSS version 20.0. Correlations were determined through Pearson’s product-moment and Spearman’s rank-order tests, with p<0.05 considered significant.
Results: The majority of participants were aged 30–39 y (44%), and females comprised 62% of the cohort. The mean SQS score was 5.2±1.1, indicating moderate sleep impairment. A strong positive correlation was found between SQS and BDI scores (r = 0.792, p<0.001), signifying that poor sleep quality was associated with greater depressive severity. Moreover, sleep quality correlated significantly with both suicidal ideation (r = 0.61, p = 0.02) and suicidal behavior (r = 0.48, p = 0.01), suggesting that deteriorating sleep quality contributes to increased suicide risk.
Conclusion: The study underscores that impaired sleep quality is intrinsically linked with depressive symptom severity and suicidality in unipolar depression. Routine evaluation and management of sleep disturbances may serve as a vital clinical strategy to improve treatment outcomes and reduce suicide vulnerability in this population.
Keywords: Unipolar depression, Sleep quality, Suicidality, PSQI, Hamilton depression rating scale
© 2026 The Authors. Published by Innovare Academic Sciences Pvt Ltd. This is an open access article under the CC BY license (https://creativecommons.org/licenses/by/4.0/)
DOI: https://dx.doi.org/10.22159/ijcpr.2026v18i1.8038 Journal homepage: https://innovareacademics.in/journals/index.php/ijcpr
INTRODUCTION
Depressive disorders represent one of the most prevalent and disabling psychiatric conditions globally, affecting approximately one in five women and one in ten men during their lifetime [1]. Despite advancements in diagnosis and treatment, these disorders continue to impose a substantial burden on affected individuals, families, and healthcare systems. Major Depressive Disorder (MDD), the prototype of unipolar depression, is characterized by pervasive low mood, anhedonia, cognitive impairment, and neurovegetative disturbances that significantly interfere with daily functioning [2]. Among these neurovegetative symptoms, disturbances in sleep are particularly common and clinically significant.
Sleep disturbance is not merely a symptom of depression but an integral component of its psychopathology, often preceding, accompanying, or persisting beyond the depressive episode [3]. Nearly 90% of patients with depression report subjective sleep complaints, including difficulty in initiating or maintaining sleep, early morning awakening, or nonrestorative sleep [4]. About two-thirds of individuals undergoing a major depressive episode experience insomnia, while hypersomnia is observed in approximately 15% [5]. Sleep problems in depression may occur as a primary manifestation, a residual symptom following treatment, or as a predictor of relapse, highlighting their clinical relevance [6]. Moreover, polysomnographic studies consistently reveal altered sleep architecture in depressed individuals, such as prolonged sleep onset latency, reduced slow-wave sleep, shortened rapid eye movement (REM) latency, and increased REM density, features considered biological markers of depression [7].
The intricate relationship between sleep quality and depressive symptomatology has been a subject of extensive investigation. Poor sleep quality contributes to heightened severity and chronicity of depressive episodes and predicts a lower response to antidepressant therapy [8]. In contrast, restoration of normal sleep patterns is often associated with symptomatic improvement and better remission rates. Furthermore, persistent sleep disturbance during remission phases has been linked to a higher risk of relapse [9]. These findings underscore that sleep quality is not only a diagnostic clue but also a prognostic determinant in unipolar depression.
Beyond its association with depressive severity, disturbed sleep has emerged as an independent risk factor for suicidality in patients with unipolar depression [10]. Suicidal behavior, encompassing suicidal ideation, planning, and attempts, constitutes a major clinical concern in depressive disorders. Approximately 15% of individuals with major depression die by suicide [11]. Recent studies have revealed that specific sleep disturbances, such as insomnia, nightmares, and fragmented sleep, significantly elevate suicidal ideation and the likelihood of suicide attempts [12]. The mechanisms linking sleep disturbance to suicidality are multifactorial, involving dysregulation of circadian rhythms, impaired emotional regulation, serotonergic dysfunction, and increased impulsivity secondary to sleep deprivation [13]. Importantly, these associations remain significant even after controlling for the severity of depressive symptoms, suggesting that sleep disruption may serve as an independent predictor of suicidal risk [14].
Given this evidence, the assessment of sleep quality assumes crucial importance in the comprehensive evaluation of patients with unipolar depression. Identifying the specific nature of sleep disturbances and understanding their interrelationship with depressive symptomatology and suicidality can aid in better risk stratification, treatment personalization, and suicide prevention strategies. While numerous international studies have explored the role of sleep in depression, there remains a paucity of systematic data in the Indian clinical context. Sociocultural factors, lifestyle variations, and differential help-seeking behaviors may influence both sleep and mood patterns, necessitating region-specific research [15].
Given the paucity of Indian studies focusing exclusively on unipolar depressive populations, this investigation seeks to elucidate the relationship between sleep quality, depressive symptom severity, and suicidality among patients diagnosed with unipolar depression. By isolating this subgroup from broader affective spectrum disorders, the study aims to provide a clearer understanding of how sleep dysregulation contributes to depressive morbidity and suicide vulnerability, thereby offering potential insights for targeted interventions in clinical practice. The research was been conducted with an objective to evaluate the relationship between sleep quality, depressive symptomatology, and suicidality among patients with unipolar depression.
MATERIALS AND METHODS
Study design
This study employed a hospital-based, cross-sectional, observational design aimed at assessing the relationship between sleep quality, depressive symptomatology, and suicidality in patients diagnosed with unipolar depression. The study was conducted among individuals fulfilling diagnostic criteria for Major Depressive Disorder as per the International Classification of Diseases, 11th Revision (ICD-11) [2].
Study setting
The study was carried out in the Department of Psychiatry, Burdwan Medical College and Hospital, Burdwan, West Bengal, India, a tertiary care teaching hospital catering to both rural and urban populations. Participants were recruited from the outpatient psychiatric services of the institution after detailed clinical evaluation.
Study duration
Data collection extended from June 2023 to June 2024. This 12 mo window ensured adequate recruitment across seasonal variations that could potentially influence sleep architecture and mood regulation.
Sampling method
Simple random sampling technique was utilized.
Sample size
50 participants suffering from unipolar depression fulfilling the below-mentioned eligibility criteria were included.
Eligibility criteria
Inclusion criteria
Participants were recruited consecutively after fulfilling the following conditions:
Age between 18 and 60 y, of either sex.
Fulfilment of diagnostic criteria for Major Depressive Disorder (Unipolar Depression) as per ICD-11, CDDR version.
Ability to understand the nature of the study and provide written, voluntary informed consent.
Adequate literacy (ability to read and write Bengali) and cognitive capacity to comprehend and respond to the administered psychometric instruments.
Drug naïve or did not take any psychotropic medications in last 2 w
Exclusion criteria
Participants were excluded if any of the following conditions were present:
Presence of intellectual disability, known organic disorder, or other psychiatric disorders (including primary sleep disorders) other than unipolar depressive disorder as per ICD-11, CDDR version.
Chronic major physical illness.
Being physically and/or psychologically too ill to be assessed for the current study.
Data collection and statistical analysis
Sociodemographic and clinical data were recorded on a pre-tested, semi-structured proforma. Diagnostic confirmation and inclusion of subjects were performed using the ICD-11, CDDR version and the Mini International Neuropsychiatric Interview (MINI) version. Sleep quality was assessed with the Sleep Quality Scale (SQS); depressive symptomatology was measured with the Bengali validated Beck Depression Inventory (BDI); and suicidality was evaluated using the Columbia-Suicide Severity Rating Scale (C-SSRS). Assessments were completed in a single session of approximately 50 min per participant.
Data were entered and analyzed using SPSS (version 20.0). Descriptive statistics (mean, standard deviation, frequency, percentage) were computed for continuous and categorical variables. Correlations between variables were examined using Pearson’s product-moment correlation (for parametric variables) and Spearman’s rank-order correlation (where appropriate). Inferential comparisons employed tests appropriate to variable type, and significance was judged at p<0.05.
Ethical clearance
The research protocol adhered to the Declaration of Helsinki (1975, revised 2000) and the synopsis was approved by the Institutional Ethics Committee (IEC) of Burdwan Medical College, Bardhaman (East); informed written, voluntary consent was obtained from all participants.
RESULTS
Sociodemographic profile
The majority of patients with unipolar depression were in the 30–39 y age group (44%), followed by 40–49 y (24%) and 20–29 y (20%). Participants aged 50 y and above constituted only 12% of the sample, indicating that unipolar depression in this cohort was more prevalent among individuals in early and middle adulthood; all these findings are being depicted in table 1.
Table 1: Age distribution of participants (n = 50)
| Age group (years) | Frequency | Percentage (%) |
| 20–29 | 10 | 20.0 |
| 30–39 | 22 | 44.0 |
| 40–49 | 12 | 24.0 |
| 50–59 | 5 | 10.0 |
| 60–69 | 1 | 2.0 |
Females predominated the sample, accounting for 62%, whereas 38% were males (fig. 2). This gender difference indicates a higher occurrence of unipolar depression among women in this study population.
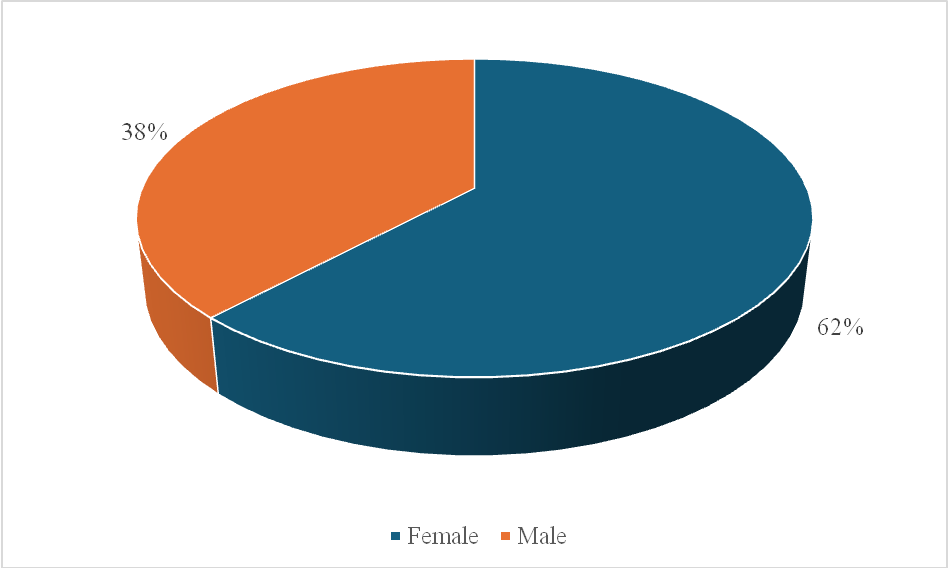
Fig. 1: Gender distribution (n = 50), the majority of participants were Hindu (48%), followed by Muslim (44%) and Christian (8%) (table 2), reflecting the general demographic composition of the study area
Table 2: Religious distribution (n = 50)
| Religion | Frequency | Percentage (%) |
| Hindu | 24 | 48.0 |
| Muslim | 22 | 44.0 |
| Christian | 4 | 8.0 |
Correlation between sleep quality cale (SQS) core and suicidal ideation/behavior
The mean sleep quality score (5.2±1.1) indicates that patients experienced moderate impairment in sleep. There was a moderate to strong positive correlation between sleep quality and both suicidal ideation (r = 0.61, p = 0.02) and suicidal behavior (r = 0.48, p = 0.01), implying that deteriorating sleep quality was associated with increased suicidal tendencies (table 3).
Table 3: Summary of core variable scores in unipolar depression (n = 50)
| Variable | Mean | Standard deviation (SD) | Statistical significance |
| Sleep Quality Scale (SQS) | 5.2 | 1.1 | – |
| Suicidal Ideation (Last Month) | r = 0.48 | p = 0.02* | Significant |
| Suicidal Behavior (Last Month) | r = 0.42 | p = 0.01* | Significant |
| Correlation: Sleep Quality × Suicidal Ideation | r = 0.61 | p = 0.02* | Significant |
| Correlation: Sleep Quality × Suicidal Behavior | r = 0.48 | p = 0.01* | Significant |
*p-value<0.05 = statistically significant.
Correlation between sleep quality and depression severity
A strong positive correlation (r = 0.792, p<0.001) was observed between Sleep Quality Scale (SQS) and Beck Depression Inventory (BDI) scores, indicating that poorer sleep quality significantly co-occurred with higher depressive severity (table 5). This suggests that as depressive symptoms intensified, the subjective sleep quality worsened proportionally.
Table 5: Correlation between sleep quality and depression severity
| Variables | r-value | p-value | Remarks |
| SQS versus BDI Scores | 0.792 | <0.001 | Strong positive correlation |
Sleep disturbance patterns
Qualitative analysis of SQS items revealed that:
High mean scores on items corresponding to sleep latency (items 6, 14) and early morning awakening (item 17) suggest prevalent difficulty in sleep initiation and maintenance.
Frequent awakenings (items 23, 26) were common and contributed to fragmented sleep continuity.
Low mean scores on items 2, 7, 8 (nightmares, sleepwalking) indicate these phenomena were relatively infrequent.
High variability (SD) in several SQS items suggests a broad range of subjective sleep disturbance severity among participants.
DISCUSSION
The present study explored the intricate interrelationship between sleep quality, depressive symptomatology, and suicidality in patients with unipolar depression. The findings highlighted a robust association between poor subjective sleep quality and both heightened depressive severity and suicidal tendencies, thereby reaffirming the fundamental role of sleep disturbance in the psychopathology of depressive disorders.
In the current study, the majority of patients with unipolar depression were within the 30–39 y age range, followed by those aged 40–49 y, reflecting the heightened vulnerability of individuals in early and middle adulthood. This age-related distribution supports the global epidemiological trend indicating that major depressive disorder (MDD) peaks during the productive adult years, coinciding with psychosocial stressors such as occupational strain, familial responsibilities, and financial burden [1].
A distinct female preponderance (62%) was observed among participants, consistent with the well-documented observation that depressive disorders occur nearly twice as frequently in women as in men [2, 3]. The underlying mechanisms are multifactorial, encompassing hormonal fluctuations across reproductive life stages, differences in hypothalamic-pituitary-adrenal (HPA) axis reactivity, and social-role-related stress exposure [4]. The present findings thus align with existing literature emphasizing the intersection of biological and psychosocial determinants in shaping the gender disparity in depression prevalence.
The present study demonstrated a strong positive correlation (r = 0.792, p<0.001) between Sleep Quality Scale (SQS) and Beck Depression Inventory (BDI) scores, indicating that poorer sleep quality corresponds with greater depressive symptom severity. This observation is congruent with prior research demonstrating that sleep disturbance is not only a symptom but a core feature and perpetuating factor in depressive episodes [3, 5].
Riemann et al. [3] and Benca et al. [4] documented consistent alterations in sleep architecture among patients with depression, including prolonged sleep latency, reduced slow-wave sleep, and shortened REM latency, all of which contribute to subjective non-restorative sleep. Similarly, Tsuno et al. [5] emphasized that these disturbances predict greater symptom chronicity and poorer treatment outcomes. The present findings corroborate this evidence, underscoring the cyclical relationship whereby depression worsens sleep quality, and poor sleep, in turn, intensifies depressive affect through dysregulation of serotonergic and circadian pathways [7].
A key observation of this study was the moderate-to-strong positive correlation between poor sleep quality and suicidal ideation (r = 0.61, p = 0.02), as well as suicidal behavior (r = 0.48, p = 0.01). These findings substantiate the growing recognition that sleep disturbances are potent, independent risk factors for suicidality in depression, irrespective of overall symptom severity.
Fawcett et al. [10] and Mann et al. [11] previously established that insomnia and nocturnal agitation are predictive of imminent suicidal behavior among depressed patients. Ağargün et al. [12] further demonstrated that patients exhibiting fragmented or poor sleep report higher suicidal ideation, while Littlewood et al. [13] qualitatively confirmed that nocturnal wakefulness magnifies feelings of hopelessness and impulsivity, mechanisms central to suicidal risk. Brüdern et al. [14] strengthened this evidence by showing that sleep disturbances predicted active suicidal ideation the following day, suggesting a temporal and potentially causal linkage.
The current study’s findings mirror these results, illustrating that impaired sleep continuity, delayed onset, and early awakening, as reflected in higher SQS scores, significantly correlated with measures of suicidality. Thus, sleep quality emerges as a clinically relevant biomarker for suicide vulnerability in unipolar depression.
The observed association between sleep disruption, depressive intensity, and suicidality may be explained through overlapping neurobiological mechanisms. Dysregulation of the serotonergic system, a central modulator of both mood and sleep, contributes to diminished REM suppression and emotional dyscontrol [7]. Furthermore, disturbed circadian rhythms and abnormal cortisol secretion patterns in depression heighten affective instability and suicidal propensity [5, 16].
This bidirectional association suggests that addressing sleep disturbance is not merely symptomatic relief but a pathophysiological intervention point. Therapeutic targeting of sleep regulation, whether through pharmacological agents acting on circadian and serotonergic systems or through non-pharmacological measures such as cognitive behavioral therapy for insomnia (CBT-I), can yield improvement in both depressive and suicidal dimensions [8, 9].
The findings of this study reinforce the importance of routinely assessing and managing sleep quality as part of a holistic approach to depression care. The incorporation of sleep hygiene education, chronotherapeutic techniques, and targeted cognitive interventions could significantly enhance clinical outcomes. Identifying poor sleepers within depressive populations may allow for early identification of patients at risk of suicidality, thereby contributing to preventive psychiatry frameworks and more precise treatment planning.
LIMITATIONS
Although the findings are consistent with international literature, certain methodological constraints must be acknowledged. The study’s cross-sectional design restricts causal inference between poor sleep and suicidality. Reliance on self-reported sleep measures rather than objective polysomnography may have introduced recall or perception bias. Moreover, the sample size was modest and confined to a single tertiary-care center, which may limit the generalizability of results. Future longitudinal studies with multimodal sleep assessments are warranted to establish directional causality and clarify underlying neurobiological mechanisms.
CONCLUSION
In conclusion, the present study underscores that sleep disturbance constitutes an integral and clinically meaningful dimension of unipolar depression. Poor sleep quality is intricately linked with greater depressive severity and heightened suicidal risk, independent of other symptom clusters. The integration of systematic sleep assessment into routine psychiatric evaluation and treatment is therefore imperative. These findings advocate for a paradigm shift toward sleep-focused interventions in the management of unipolar depression, with potential to mitigate relapse, reduce suicidality, and enhance overall treatment efficacy.
ACKNOWLEDGMENT
The authors express his sincere gratitude to the Department of Psychiatry, Burdwan Medical College and Hospital, for providing the facilities and support necessary to complete this research work.
FUNDING
This study was entirely self-funded.
AUTHORS CONTRIBUTIONS
Dr. Roy conceptualized the study, designed the methodology, collected clinical data, performed the statistical analysis and critically reviewed the manuscript; Dr. Das has supervised the research, reconfirmed the analysis, and contributed substantially to writing and approved the final manuscript.
CONFLICT OF INTERESTS
There are no conflict of interests in this research.
REFERENCES
World Health Organization. Mental health: strengthening our response. Geneva; 2019. Available from: https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response.
World Health Organization. Clinical descriptions and diagnostic requirements for ICD-11 mental, behavioural and neurodevelopmental disorders. Geneva; 2024. Available from: https://www.who.int/publications/i/item/9789240077263. [Last accessed on 21 Oct 2025].
Riemann D, Berger M, Voderholzer U. Sleep and depression results from psychobiological studies: an overview. Biol Psychol. 2001 Jul-Aug;57(1-3):67-103. doi: 10.1016/s0301-0511(01)00090-4, PMID 11454435.
Benca RM, Obermeyer WH, Thisted RA, Gillin JC. Sleep and psychiatric disorders. A meta-analysis. Arch Gen Psychiatry. 1992 Aug;49(8):651-68. doi: 10.1001/archpsyc.1992.01820080059010, PMID 1386215.
Tsuno N, Besset A, Ritchie K. Sleep and depression. J Clin Psychiatry. 2005 Oct;66(10):1254-69. doi: 10.4088/JCP.v66n1008, PMID 16259539.
Cho HJ, Lavretsky H, Olmstead R, Levin MJ, Oxman MN, Irwin MR. Sleep disturbance and depression recurrence in community-dwelling older adults: a prospective study. Am J Psychiatry. 2008 Dec;165(12):1543-50. doi: 10.1176/appi.ajp.2008.07121882, PMID 18765482.
Armitage R. Sleep and circadian rhythms in mood disorders. Acta Psychiatr Scand Suppl. 2007;(433):104-15. doi: 10.1111/j.1600-0447.2007.00968.x, PMID 17280576.
Nierenberg AA, Keefe BR, Leslie VC, Alpert JE, Pava JA, Worthington JJ. Residual symptoms in depressed patients who respond acutely to fluoxetine. J Clin Psychiatry. 1999 Apr;60(4):221-5. doi: 10.4088/JCP.v60n0403, PMID 10221281.
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989 May;28(2):193-213. doi: 10.1016/0165-1781(89)90047-4, PMID 2748771.
Fawcett J, Scheftner WA, Fogg L, Clark DC, Young MA, Hedeker D. Time-related predictors of suicide in major affective disorder. Am J Psychiatry. 1990 Sep;147(9):1189-94. doi: 10.1176/ajp.147.9.1189, PMID 2104515.
Mann JJ, Apter A, Bertolote J, Beautrais A, Currier D, Haas A. Suicide prevention strategies: a systematic review. JAMA. 2005 Oct 26;294(16):2064-74. doi: 10.1001/jama.294.16.2064, PMID 16249421.
Agargun MY, Kara H, Solmaz M. Sleep disturbances and suicidal behavior in patients with major depression. J Clin Psychiatry. 1997 Jun;58(6):249-51. doi: 10.4088/JCP.v58n0602, PMID 9228889.
Littlewood DL, Gooding P, Kyle SD, Pratt D, Peters S. Understanding the role of sleep in suicide risk: qualitative interview study. BMJ Open. 2016 Aug 22;6(8):e012113. doi: 10.1136/bmjopen-2016-012113, PMID 27550652.
Brudern J, Hallensleben N, Huller I, Spangenberg L, Forkmann T, Rath D. Sleep disturbances predict active suicidal ideation the next day: an ecological momentary assessment study. BMC Psychiatry. 2022 Jan 27;22(1):65. doi: 10.1186/s12888-022-03716-6, PMID 35086519.
Livingston G, Blizard B, Mann A. Does sleep disturbance predict depression in elderly people? A study in inner London. Br J Gen Pract. 1993 Nov;43(376):445-8. PMID 8292414.
Wulff K, Gatti S, Wettstein JG, Foster RG. Sleep and circadian rhythm disruption in psychiatric and neurodegenerative disease. Nat Rev Neurosci. 2010 Aug;11(8):589-99. doi: 10.1038/nrn2868, PMID 20631712.