
Int J Curr Pharm Res, Vol 18, Issue 1, 121-125Original Article
QUALITY OF SLEEP AND ITS RELATIONSHIP WITH DEPRESSIVE SYMPTOMATOLOGY AND SUICIDALITY IN BIPOLAR DEPRESSION
BHASKAR ROY1, PRANAB DAS2*
1Department of Psychiatry, Burdwan Medical College and Hospital, Bardhaman, West Bengal, India. 2Department of Pharamacology, Pragjyotishpur Medical College and Hospital, Guwahati, Assam, India
*Corresponding author: Pranab Das; *Email: pranabdas2580123@gmail.com
Received: 10 Oct 2025, Revised and Accepted: 27 Nov 2025
ABSTRACT
Objective: To evaluate the relationship between sleep quality, depressive symptomatology, and suicidality among patients with bipolar depression.
Methods: This hospital-based, cross-sectional observational study was conducted in the Department of Psychiatry, Burdwan Medical College and Hospital, West Bengal. Fifty participants fulfilling ICD-11 diagnostic criteria for bipolar affective disorder in the depressive phase were enrolled using simple random sampling. Standardized instruments were applied like Sleep Quality Scale (SQS) to assess subjective sleep parameters, Beck Depression Inventory (BDI) to quantify depressive severity, and Columbia–Suicide Severity Rating Scale (C-SSRS) to evaluate suicidality. Statistical analysis was performed using SPSS version 20.0, employing Pearson’s and Spearman’s correlation coefficients, with significance set at p<0.05.
Results: Participants demonstrated moderate sleep impairment (mean SQS score = 4.9±1.2) and significant depressive symptoms. A strong positive correlation was observed between SQS and BDI scores (r = 0.846, p<0.001), indicating that poorer sleep quality was associated with greater depressive severity. Sleep quality also correlated moderately with suicidal ideation (r = 0.49, p = 0.01) and suicidal behavior (r = 0.54, p = 0.01), underscoring the independent contribution of sleep disturbance to suicidality.
Conclusion: Sleep dysfunction constitutes a pivotal element in the psychopathology of bipolar depression, strongly influencing both mood intensity and suicidal risk. Integrating systematic sleep evaluation and targeted interventions such as circadian rhythm regulation and behavioral sleep therapy into routine management may enhance clinical outcomes and mitigate suicidal vulnerability in bipolar depressive patients.
Keywords: Bipolar depression, Sleep quality, Suicidality, PSQI, Hamilton depression rating scale
© 2026 The Authors. Published by Innovare Academic Sciences Pvt Ltd. This is an open access article under the CC BY license (https://creativecommons.org/licenses/by/4.0/)
DOI: https://dx.doi.org/10.22159/ijcpr.2026v18i1.8051 Journal homepage: https://innovareacademics.in/journals/index.php/ijcpr
INTRODUCTION
Bipolar depression constitutes a significant public health challenge characterized by recurrent episodes of mood disturbance alternating between mania or hypomania and depression. Despite therapeutic advancements, bipolar disorder remains one of the most disabling psychiatric illnesses, often associated with impaired psychosocial functioning, reduced quality of life, and heightened suicide risk. According to the World Health Organization (WHO), bipolar disorder affects approximately 1% of the global population, while the broader bipolar spectrum disorders affect about 2.4%, with equal gender distribution in bipolar I disorder and female predominance in bipolar II disorder [1, 2]. The age of onset typically occurs in early adulthood, with men exhibiting earlier onset than women, reflecting distinct biological and psychosocial vulnerabilities across subtypes.
Sleep disturbances are pervasive across all phases of bipolar disorder. During depressive episodes, patients frequently experience insomnia, hypersomnia, or circadian rhythm disruption, contributing to emotional dysregulation and cognitive impairment [3, 4]. Studies have demonstrated that up to 90% of individuals with mood disorders report altered sleep quality, with sleep-onset insomnia and early morning awakening being particularly pronounced during bipolar depression [5]. Conversely, hypersomnia has been associated with atypical depressive features, further complicating diagnostic clarity [6]. These disruptions not only represent symptomatic dimensions but also serve as markers of illness activity, relapse, and suicidal behavior.
The relationship between sleep quality, depressive symptomatology, and suicidality in bipolar depression is both intricate and clinically consequential. Sleep deprivation can exacerbate affective instability, precipitate manic switches, and increase impulsivity, thereby heightening suicidal tendencies [7, 8]. Moreover, disrupted sleep architecture involving reduced slow-wave sleep and shortened REM latency has been linked to poor emotional regulation and elevated suicidality among individuals with bipolar disorder [9]. Understanding this triadic association is crucial, as sleep dysfunction may represent a modifiable therapeutic target for improving mood stability and reducing suicide risk.
The current study was undertaken with an objective to systematically assess sleep quality and its correlation with depressive severity and suicidality among patients with bipolar depression. Given that most literature has focused on unipolar depression, this investigation aimed to bridge a critical gap by elucidating the role of sleep pathology within the bipolar depressive spectrum, thereby offering insights for early intervention and comprehensive clinical management.
MATERIALS AND METHODS
Study design
The present investigation adopted a hospital-based, observational cross-sectional design, aimed at exploring the interrelationship between sleep quality, depressive symptomatology, and suicidality among patients diagnosed with bipolar depression. The study focused exclusively on individuals fulfilling the ICD-11 clinical diagnostic criteria for bipolar affective disorder in the depressive phase [2].
Study setting
The research was conducted in the Department of Psychiatry, Burdwan Medical College and Hospital (BMCH), located in Burdwan, West Bengal, India, which is a tertiary care institution providing psychiatric services to a large catchment area encompassing both urban and rural populations. Participants were recruited from outpatient psychiatric units, ensuring a representative clinical sample.
Study duration
The total study duration was one year (June 2023 to June 2024), which included the phases of patient recruitment, data collection, data analysis, and manuscript preparation.
Sampling method
A simple random sampling technique was employed to select participants from among patients attending the psychiatry outpatient department of BMCH.
Sample size
50 participants suffering from bipolar depression satisfying the below-mentioned eligibility criteria were included.
Eligibility criteria
Inclusion criteria
Participants were included in the study if they met the following criteria:
Age ranging from 18 to 60 years, of either sex.
Fulfilled the ICD-11 CDDR diagnostic criteria for Bipolar affective disorder, depressive episode.
Provided written, voluntary informed consent after being briefed about the study’s purpose and procedures.
Were literate and able to read and write in Bengali to ensure valid comprehension of assessment tools.
Were either drug-naïve or had not received any psychotropic medication for at least two weeks prior to assessment.
Exclusion criteria
Participants were excluded if they met any of the following conditions:
Presence of intellectual disability, organic brain syndrome, or other psychiatric disorders (including primary sleep disorders) apart from bipolar depression.
Presence of chronic physical illnesses (e. g., hypothyroidism, diabetes, cardiovascular or neurological disorders) likely to influence mood or sleep regulation.
Patients who were severely ill or uncooperative rendering them unable to complete the required assessment scales.
Data collection and statistical analysis
After obtaining voluntary, informed and written consent, each participant was evaluated using a pre-validated, semi-structured sociodemographic and clinical data sheet prepared specifically for the study. Diagnostic confirmation was carried out by using ICD-11 CDDR diagnostic criteria for bipolar affective disorder (depressive episode) and Mini International Neuropsychiatric Interview (MINI 5.0.0), ensuring diagnostic reliability.
The following standardized psychometric instruments were administered:
Sleep Quality Scale (SQS): To evaluate subjective sleep quality and associated disturbances.
Beck Depression Inventory (BDI): To assess the severity of depressive symptomatology.
Columbia–Suicide Severity Rating Scale (C-SSRS): To evaluate suicidal ideation and suicidal behavior over the preceding month.
Each assessment was conducted in a single session of approximately 50 min, in a quiet clinical environment to minimize external interference.
Data were entered and statistically analyzed using the Statistical Package for the Social Sciences (SPSS) software, version 20.0. Descriptive statistics such as mean, standard deviation, and percentage were calculated for quantitative and categorical variables. Relationships between sleep quality, depression severity, and suicidality were analyzed using Pearson’s product–moment correlation and Spearman’s rank correlation coefficient as appropriate. Significance was established at a p-value<0.05.
Ethical clearance
The study protocol received prior approval from the Institutional Ethics Committee (IEC) of BMCH, Burdwan, West Bengal. All participants were briefed about the study and provided written informed consent in their native language before participation. The research adhered to the ethical principles outlined in the Declaration of Helsinki (2013 revision) and complied with institutional and national ethical guidelines governing human research.
RESULTS
Sociodemographic profile
In the bipolar depression group (n = 50), the majority of participants were aged 30–39 years (34%), followed by 20–29 years (24%) and 40–49 years (18%). Only 2% of participants were aged 70 years or above, indicating a higher prevalence of depressive episodes in early to middle adulthood (table 1).
Females (56%) outnumbered males (44%), suggesting a gender pattern consistent with prior studies showing greater depressive polarity among women in bipolar affective disorder (fig. 2).
In terms of religion, Hindus constituted 58%, Muslims 36%, and Christians 6%, broadly reflecting the demographic composition of the region (table 2). The majority were married (84.31%), and most had education upto mid-school or are illiterate (30%), highlighting that bipolar depressive morbidity affects individuals across diverse social and educational backgrounds.
These findings indicate that bipolar depression was most prevalent among adult females in their thirties, paralleling global observations of gender and age distribution trends in mood disorders.
Table 1: Age distribution of participants with bipolar depression (n = 50)
| Age group (years) | Frequency | Percentage (%) |
| 20–29 | 12 | 24.0 |
| 30–39 | 17 | 34.0 |
| 40–49 | 9 | 18.0 |
| 50–59 | 6 | 12.0 |
| 60–69 | 5 | 10.0 |
| >70 | 1 | 2 |
Table 2: Religious distribution with bipolar depression (n = 50)
| Religion | Frequency | Percentage (%) |
| Hindu | 29 | 58.0 |
| Muslim | 18 | 36.0 |
| Christian | 3 | 6.0 |
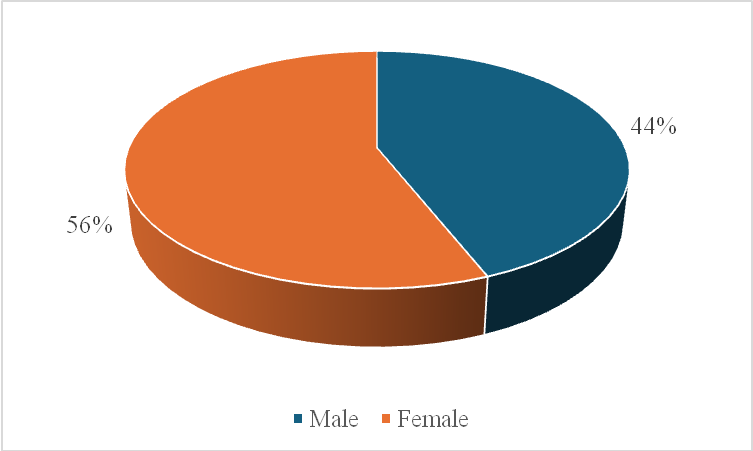
Fig. 1: Gender distribution with bipolar depression (n = 50)
Clinical and psychometric findings
Sleep disturbance patterns
Participants demonstrated significant depressive symptomatology and moderate sleep impairment. The mean Sleep Quality Scale (SQS) score was 4.9±1.2, reflecting moderate subjective sleep disturbance.
Item-wise analysis of the Sleep Quality Scale (SQS) indicated that the most disturbed domains included:
High mean Scores on Items 18, 13, 2, and 6 suggests insomnia, fragmented sleep, and difficulty staying asleep.
Low mean Scores on Items 8, 3, and 12 indicates that certain sleep issues (like nightmares) are not universal in bipolar disorder.
High Standards Deviation (SD) in Items 12, 9, and 24 suggests that some patients experience extreme sleep issues, while others do not, possibly due to mood phases.
Correlation between sleep quality and depression severity
A detailed correlational analysis between the Sleep Quality Scale (SQS) and the Beck Depression Inventory (BDI) scores among patients with bipolar depression (n = 50) revealed a strong, statistically significant positive correlation (r = 0.846, p<0.001) (table 3). This finding implies that as subjective sleep quality deteriorated, the intensity of depressive symptomatology increased in a nearly proportional manner.
The strong correlation suggests a bidirectional relationship: disturbed sleep exacerbates depressive symptoms through mechanisms such as altered REM architecture and hyperarousal, while depression further disrupts sleep through dysregulation of melatonin and cortisol rhythms. Clinically, this emphasizes the need for comprehensive sleep evaluation and management in the treatment of bipolar depression, as improving sleep may meaningfully attenuate depressive intensity and stabilize mood states.
Table 3: Summary of correlation between sleep quality and depression severity in bipolar depression (n = 50)
| Variable Pair | Correlation (r) | p-value | Significance | Interpretation |
| Sleep Quality Scale × Beck Depression Inventory | 0.846 | <0.001 | Highly Significant | Strong positive correlation: poorer sleep associated with greater depressive severity |
Correlation between sleep quality and suicidality
A subsequent analysis examined the association between sleep quality and suicidal ideation and suicidal behavior as measured by the Columbia-Suicide Severity Rating Scale (C-SSRS). Results demonstrated moderate but statistically significant positive correlations between SQS and suicidal ideation (r = 0.49, p = 0.01) and between SQS and suicidal behavior (r = 0.54, p = 0.01). These values indicate that individuals with poorer sleep quality were more likely to experience persistent suicidal thoughts and to engage in suicidal acts. These findings highlight that worsening sleep quality significantly amplifies suicidal ideation and behavior, independent of depressive symptom severity.
Table 4: Correlation between sleep quality and depression severity
| Variable pair | Correlation (r) | p-value | Significance | Interpretation |
| Sleep Quality × Suicidal Ideation | 0.49 | 0.01 | Significant | Poorer sleep associated with increased suicidal thoughts |
| Sleep Quality × Suicidal Behavior | 0.54 | 0.01 | Significant | Worse sleep linked to greater suicidal actions |
DISCUSSION
The present study explored the intricate association between sleep quality, depressive symptomatology, and suicidality in patients with bipolar depression. The findings revealed a strong and statistically significant positive correlation between sleep disturbance and depressive severity (r = 0.846, p<0.001), and moderate significant correlations between sleep quality and suicidality: both suicidal ideation (r = 0.49, p = 0.01) and suicidal behavior (r = 0.54, p = 0.01). These results underscore the multifaceted role of sleep dysregulation as both a marker and a mediator of affective instability and suicidal vulnerability in bipolar depression.
In the bipolar subgroup, depressive episodes were most prevalent among adults aged 30–39 years, followed by those in the 20–29 y bracket, consistent with epidemiological findings indicating that bipolar affective disorder often manifests in early adulthood and continues to exert episodic recurrence across the lifespan [10]. This age clustering corresponds with the stress-vulnerability model, which implicates occupational stressors, social role transitions, and circadian disruption during productive adult years as potential triggers for mood destabilization.
The female preponderance (56%) observed in the present study aligns with prior global evidence suggesting higher rates of depressive polarity among women diagnosed with bipolar disorder. Hormonal fluctuations, neuroendocrine sensitivity to stress, and psychosocial role demands have been proposed as contributing factors [11, 12]. These findings collectively support the biopsychosocial framework underlying gender differences in mood disorder presentation.
The strong positive correlation between SQS and BDI scores (r = 0.846, p<0.001) signifies that worsening subjective sleep quality parallels an increase in depressive symptom intensity. Similar observations were reported by Brüdern et al. (2022), who found that day-to-day variations in sleep quality predicted next-day depressive affect [13]. Wilson et al. (2020) further demonstrated that impaired sleep continuity significantly reduced antidepressant response efficacy, emphasizing the bidirectional influence of sleep and mood regulation [14].
Pathophysiologically, this relationship may reflect disturbances in circadian rhythm synchronization and monoaminergic neurotransmission, particularly serotonergic and dopaminergic pathways, which regulate both sleep architecture and affective tone [8]. Wehr et al. (1987) previously hypothesized that sleep reduction could precipitate manic or mixed episodes by altering REM latency and triggering neurobiological overactivation. Within the depressive polarity, however, such disturbances tend to perpetuate fatigue, cognitive dulling, and emotional dysregulation. The present findings thus align with established evidence that poor sleep quality is not merely symptomatic but constitutive of the depressive process in bipolar disorder [8].
A pivotal observation of this study was the significant correlation between poor sleep quality and suicidal ideation and behavior. The coefficients (r = 0.49 and r = 0.54, respectively) reflect moderate-to-strong associations, suggesting that sleep impairment operates as an independent risk factor for suicidality in bipolar depression, beyond the influence of general depressive severity.
This observation finds strong support in prior literature. Ağargün et al. (1997) demonstrated that suicidal patients with depression exhibited markedly worse sleep quality compared to non-suicidal counterparts [15]. Similarly, Littlewood et al. (2016), using qualitative methods, revealed that nocturnal wakefulness fosters intrusive thoughts, hopelessness, and emotional dyscontrol, all of which contribute to suicidal intent [16]. Brüdern et al. (2022) corroborated this through an ecological momentary assessment, showing that sleep disturbances predicted next-day active suicidal ideation [13].
Mechanistically, sleep deprivation and fragmentation are thought to heighten impulsivity and affective lability by dysregulating prefrontal cortical inhibition and serotonergic tone, both implicated in suicidal risk. Moreover, nighttime wakefulness removes individuals from social and environmental buffers, allowing ruminative cognition to dominate [17]. Therefore, routine assessment of sleep patterns may serve as an early clinical indicator of suicidal risk in bipolar populations.
The stronger SQS–BDI correlation in bipolar depression (r = 0.846) relative to unipolar depression (r = 0.792) in this thesis suggests that sleep disruption exerts a more pronounced impact on mood stability in bipolar disorder. Previous research has identified sleep disturbance as both a prodromal symptom and a precipitant of bipolar episodes, with abnormal circadian rhythms serving as a core trait marker [7, 18]. Harvey (2008) emphasized that targeting circadian misalignment could significantly improve mood outcomes and reduce relapse risk [7].
Additionally, studies such as Pegion et al. (2008) and Daniel et al. (Zurich Study, 2003) demonstrated that persistent insomnia predicted both the onset and chronicity of mood episodes, further validating sleep as a therapeutic target [19, 20]. The current study’s findings resonate with these results, reinforcing the premise that stabilizing sleep may attenuate affective intensity and suicidality in bipolar depression.
The present study possesses several noteworthy strengths. First, it employed standardized and psychometrically validated instruments, namely, the Sleep Quality Scale (SQS), Beck Depression Inventory (BDI), and Columbia–Suicide Severity Rating Scale (C-SSRS), which ensured reliable quantification of sleep quality, depressive severity, and suicidality. Second, by focusing exclusively on bipolar depression, the study contributes to a relatively underexplored domain where most prior research has emphasized unipolar affective disorders. Third, the use of a well-defined hospital-based sample and rigorous diagnostic confirmation using ICD-11 criteria enhanced the internal validity of findings. Furthermore, the statistical analysis was robust, establishing significant and clinically meaningful correlations that underscore the interconnectedness of sleep disturbances, affective symptomatology, and suicidal risk. The inclusion of qualitative item-level SQS interpretation added depth by revealing specific domains of sleep dysfunction characteristic of bipolar depression.
From a clinical perspective, the findings underscore the need for integrated sleep assessment in the management of bipolar depression. Given the demonstrated association between sleep disturbance, depression severity, and suicidality, incorporating behavioral sleep interventions, circadian rhythm therapy, and sleep hygiene counseling could enhance overall treatment efficacy. Furthermore, sleep-focused interventions could function as early preventive strategies against suicidal escalation, particularly in patients presenting with insomnia-type symptoms.
LIMITATIONS
Despite these strengths, certain limitations must be acknowledged. The study employed a cross-sectional design, which restricts causal inference regarding the directionality of the observed relationships. Longitudinal follow-up could better delineate whether poor sleep precedes worsening depression or vice versa. The sample size, though adequate for correlation analysis, limits the generalizability of the findings beyond similar tertiary-care clinical settings. The study also relied on self-reported sleep quality measures, which may be subject to recall bias and subjective variability. Objective assessments such as polysomnography or actigraphy were not utilized, potentially underestimating certain physiological aspects of sleep disturbance. Lastly, although suicidality was comprehensively evaluated, biological and psychosocial covariates such as medication history, duration of illness, or comorbid anxiety were not statistically controlled, warranting further exploration in future research.
CONCLUSION
This study highlights the central role of sleep quality in shaping depressive symptomatology and suicidality among individuals with bipolar depression. A strong positive correlation (r = 0.846, p<0.001) was observed between sleep disturbance and depression severity, while moderate significant correlations emerged between poor sleep and suicidal ideation (r = 0.49, p = 0.01) and suicidal behavior (r = 0.54, p = 0.01). These findings affirm that sleep dysfunction is not merely an ancillary symptom but a critical component of the bipolar depressive phenotype, influencing both affective burden and suicide risk. Clinically, the results emphasize the importance of routine sleep assessment as an integral part of psychiatric evaluation. Targeting sleep regulation through behavioral interventions, circadian rhythm therapies, and pharmacologic modulation could substantially enhance mood stabilization and reduce suicidality. Future studies incorporating objective sleep measures, larger samples, and longitudinal designs are warranted to deepen understanding and improve patient outcomes.
ACKNOWLEDGMENT
The authors extend their sincere gratitude to all the patients and their families who participated in this study for their valuable time and cooperation. We are deeply thankful to the faculty and postgraduate residents of the Department of Psychiatry, Burdwan Medical College and Hospital, for their assistance during data collection and patient evaluation. Special appreciation is due to the Institutional Ethics Committee of Burdwan Medical College, whose guidance ensured ethical compliance throughout the research process.
FUNDING
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
AUTHORS CONTRIBUTIONS
Dr. Roy conceived the study design, conducted literature review, performed data collection, statistical analysis, and manuscript drafting; Dr. Das has contributed to the interpretation of results, and critically reviewed the final manuscript for academic accuracy and coherence.
CONFLICT OF INTERESTS
The authors declare no conflicts of interest related to this research, authorship, or publication of this manuscript.
REFERENCES
World Health Organization. Mental health: strengthening our response. Geneva: World Health Organization; 2019. Available from: https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response. [Last accessed on 31 Dec 2025].
World Health Organization. ICD-11 clinical descriptions and diagnostic guidelines for mental and behavioural disorders. Geneva: World Health Organization; 2022. Available from: https://www.who.int/publications/i/item/9789240077263. [Last accessed on 21 Oct 2025].
Riemann D, Berger M, Voderholzer U. Sleep and depression results from psychobiological studies: an overview. Biol Psychol. 2001 Jul-Aug;57(1-3):67-103. doi: 10.1016/S0301-0511(01)00090-4, PMID 11454435.
Armitage R. Sleep and circadian rhythms in mood disorders. Acta Psychiatr Scand Suppl. 2007;(433):104-15. doi: 10.1111/j.1600-0447.2007.00968.x, PMID 17280576.
Tsuno N, Besset A, Ritchie K. Sleep and depression. J Clin Psychiatry. 2005 Oct;66(10):1254-69. doi: 10.4088/JCP.v66n1008, PMID 16259539.
Kaplan KA, Harvey AG. Hypersomnia across mood disorders: a review and synthesis. Sleep Med Rev. 2009 Aug;13(4):275-85. doi: 10.1016/j.smrv.2008.09.001, PMID 19269201.
Harvey AG. Sleep and circadian rhythms in bipolar disorder: seeking synchrony harmony and regulation. Am J Psychiatry. 2008 Jul;165(7):820-9. doi: 10.1176/appi.ajp.2008.08010098, PMID 18519522.
Wehr TA, Sack DA, Rosenthal NE. Sleep reduction as a final common pathway in the genesis of mania. Am J Psychiatry. 1987 Feb;144(2):201-4. doi: 10.1176/ajp.144.2.201, PMID 3812788.
Plante DT, Winkelman JW. Sleep disturbance in bipolar disorder: therapeutic implications. Am J Psychiatry. 2008 Jul;165(7):830-43. doi: 10.1176/appi.ajp.2008.08010077, PMID 18483132.
Garcia Velazquez R, Jokela M, Rosenstrom TH. The varying burden of depressive symptoms across adulthood: results from six NHANES cohorts. J Affect Disord. 2019 Mar 1;246:290-9. doi: 10.1016/j.jad.2018.12.059, PMID 30594042.
Salk RH, Hyde JS, Abramson LY. Gender differences in depression in representative national samples: meta-analyses of diagnoses and symptoms. Psychol Bull. 2017 Aug;143(8):783-822. doi: 10.1037/bul0000102, PMID 28447828.
Blazer DG. Depression in late life: review and commentary. J Gerontol A Biol Sci Med Sci. 2003 Mar;58(3):249-65. doi: 10.1093/gerona/58.3.M249, PMID 12634292.
Brudern J, Hallensleben N, Holler I, Spangenberg L, Forkmann T, Rath D. Sleep disturbances predict active suicidal ideation the next day: an ecological momentary assessment study. BMC Psychiatry. 2022 Jan 27;22(1):65. doi: 10.1186/s12888-022-03716-6, PMID 35086519.
Wilson S, Argyropoulos S. Antidepressants and sleep: a qualitative review of the literature. Drugs. 2005;65(7):927-47. doi: 10.2165/00003495-200565070-00003, PMID 15892588.
Agargun MY, Kara H, Solmaz M. Sleep disturbances and suicidal behavior in patients with major depression. J Clin Psychiatry. 1997 Jun;58(6):249-51. doi: 10.4088/JCP.v58n0602, PMID 9228889.
Littlewood DL, Gooding P, Kyle SD, Pratt D, Peters S. Understanding the role of sleep in suicide risk: qualitative interview study. BMJ Open. 2016 Aug 22;6(8):e012113. doi: 10.1136/bmjopen-2016-012113, PMID 27550652.
Perlis ML, Grandner MA, Brown GK, Basner M, Chakravorty S, Morales KH. Nocturnal wakefulness as a previously unrecognized risk factor for suicide. J Clin Psychiatry. 2016 Jun;77(6):e726-33. doi: 10.4088/JCP.15m10131, PMID 27337421.
Kaplan KA, Harvey AG. Hypersomnia across mood disorders: a review and synthesis. Sleep Med Rev. 2009 Aug;13(4):275-85. doi: 10.1016/j.smrv.2008.09.001, PMID 19269201.
Pigeon WR, Hegel M, Unutzer J, Fan MY, Sateia MJ, Lyness JM. Is insomnia a perpetuating factor for late-life depression in the Impact cohort? Sleep. 2008 Apr;31(4):481-8. doi: 10.1093/sleep/31.4.481, PMID 18457235.
Taylor DJ. Insomnia and depression. Sleep. 2008 Apr;31(4):447-8. doi: 10.1093/sleep/31.4.447, PMID 18457230.